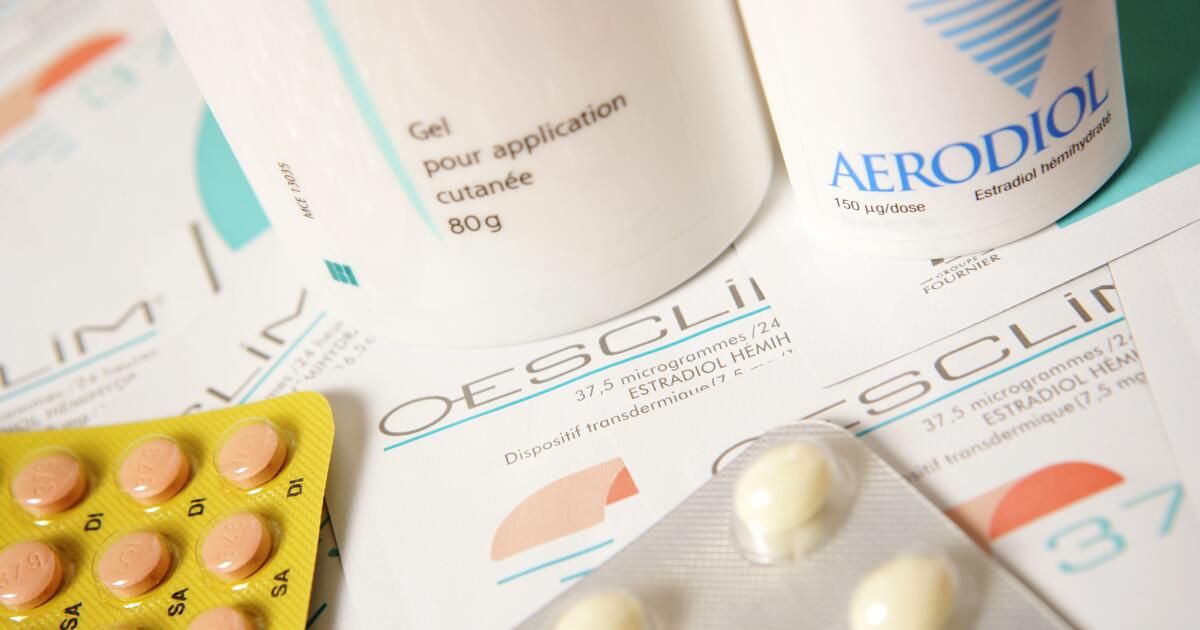
For months now, menopausal women across the United States have been unable to fill prescriptions for the estradiol patch, a safe and long-standing hormone treatment. The media has sparked a frenzy over this shortage, warning of a long lasting national shortage. The problem is real, but the explanations in media coverage miss the mark. Real solutions depend on an accurate understanding of the causes.
Reporters, pharmaceutical companies and even some doctors have blamed women for causing the shortages, saying they were inspired by a “menopause time“which has promoted unprecedented demand. This framework dangerously harms the essential defense of health.
In this narrativeThere has been unprecedented demand, and it is partly explained by the Food and Drug Administration's recent removal of the “black box warning” from the packaging of estradiol patches. That inaccurate (and, frankly, scary) label had been necessary since a 2002 ad exaggerated the link between certain menopausal hormone treatments and breast cancer. It is long overdue to correct the size and rephrase the warning. But the problem with this narrative is that even after the black box warning was removed, there has been unprecedented demand.
Around 40% of menopausal women were prescribed some form of hormone treatment before the 2002 announcement. Use plummeted afterward, dropping to less than 5% in 2020 and only 1.8% in 2024. According to the most recent datathe figure has now stabilized at the 5% mark. Unprecedented? Hardly. Modest at best.
Estradiol is also not a new or complex drug; The patch formulation has been around for decades and generic versions are widely manufactured. There's no exotic ingredient, no weird supply chain dependency, no coincidence that explains why women are suddenly told their pharmacy is out of stock month after month.
The story is much more a critique of the failed insurance industry: market concentration, perverse incentives, and the consequences of allowing insurance companies to own the pharmacy benefit managers that effectively control access to medications for most users. three companies – CVS Caremark, Express Scripts and OptumRx: handle 79% of all prescription drug claims in the United States. Those companies are wholly owned subsidiaries of three insurance giants: CVS Health, Cigna and UnitedHealth Group, respectively. This means that the same corporation that sells you your insurance plan also decides what medications are covered, at what price, and whether your pharmacy can stock them. This is called vertical integration. In another era, we could have called it a poster. The resulting problems are not unique to hormonal treatments; have affected widely used medicines, including anticoagulants, inhalers and antibiotics. When a low-cost generic like estradiol (a blockbuster, no-margin drug without patent protection) conflicts in this system, the friction is not random. It is structural. Every decision in that chain is filtered through the same corporate profit motive. And when the drug in question is an off-patent estradiol patch that has negligible profit margins due to generic competition but requires logistical investment to keep it in stock consistently? The math on “how much this company cares about ensuring access” isn't complicated.
Unfortunately, there are few financial incentives to ensure smooth and consistent access. However, there is a significant financial incentive to steer patients toward brand-name alternatives, or simply let supply decline, because companies are not losing much profit if sales of that product decline. This Isn't a Conspiracy Theory: The Federal Trade Commission Noticed This Dynamic in a report which documented how pharmacy benefit managers' practices inflate costs, reduce competition, and harm patient access, particularly for independent pharmacies and generic drugs.
Any claim that the shortage of estradiol patches is significantly due to more women now demanding hormonal treatments is a distraction. It is also misogyny, pure and simple, to imply that the solution to the shortage is for women's health advocates to reduce it and for women to moderate their expectations. The shortage of estradiol patches is the result of a broken system that refuses to provide an adequate supply.
In the meantime, there are some strategies to deal with it.
- Ask your doctor about alternatives. Estradiol is available in multiple formulations, including gel, spray, cream, oral tablet, vaginal ring, and weekly transdermal patch, which is a different product from the twice-weekly patch and may be available more consistently depending on the manufacturer and region.
- Consider a online pharmacy. Many are doing a good job locating and filling these prescriptions from outside the pharmacy benefit management system.
- Call ahead. Patch shortages are inconsistent between regions and distributors. A call to pharmacies in your area, or a wider geographic radius if you can, can locate stock that your regular pharmacy doesn't carry.
- Consider a compounding pharmacy. These sources can sometimes meet needs when commercially manufactured products are inaccessible. The hormones used are the same bulk ingredients regulated by the FDA.
Beyond those stopgap solutions, more Americans need to fight for systemic change. The FTC report exists because Congress requested it and committed to legislation which will solve at least some of the problems. The FDA moved to change estrogen labeling under pressure from citizens and medical experts; should do more now to demand transparency from patch manufacturers.
Most importantly, it is up to all of us to call out the flaws in the current system. Instead of repeating “there is a shortage of patches” or “increasing demand”, let's say that a surprisingly small minority of menopausal women are still prescribed hormone treatments, and that three pharmaceutical companies control the vast majority of claims in this country. Those are real problems that need real solutions.
Jennifer Weiss-Wolf, executive director of the Birnbaum Women's Leadership Center at New York University School of Law, is the author of the upcoming book. “When you are in menopause: user manual and citizen's guide.“ Suzanne Gilberg, an OB-GYN in Los Angeles, is the author of “Menopause Bootcamp.”